What are uterine fibroids?
Uterine fibroids are tumors or growths, made up of muscle cells and other tissues that grow within the wall of the uterus (or womb). Although fibroids are sometimes called tumors, they are almost always benign (not cancerous). The medical term for fibroids is uterine leiomyomata (pronounced you-ter-in lie-oh-my-oh-mah-tah). Fibroids can grow as a single growth or in clusters (or groups). Their size can vary from small, like an apple seed (or less than one inch), to even larger than a grapefruit, or eight inches across or more.
Background
Why should women know about fibroids?
Uterine fibroids are the most common benign tumors in women of childbearing age, but no one knows exactly what causes them. They can be frustrating to live with because there are limited treatment options, and they are the cause of many hysterectomies (surgery to remove the uterus).
Where can fibroids grow?
Fibroids are placed into three groups based on where they grow, such as just underneath the lining of the uterus, in between the muscles of the uterus, or on the outside of the uterus. Most fibroids grow within the wall of the uterus. Some fibroids grow on stalks (called peduncles) that grow out from the surface of the uterus, or into the cavity of the uterus.
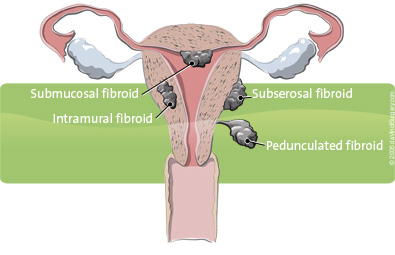
What are the symptoms of fibroids?
Most fibroids do not cause any symptoms, but some women with fibroids can have:
- Heavy bleeding or painful periods
- Bleeding between periods
- Feeling of fullness in the pelvic area (lower abdomen)
- Urinating often
- Pain during sex
- Lower back pain
- Reproductive problems - such as infertility, having more than one miscarriage, or having early onset of labor during pregnancy
What our patients say:
Uterine Fibroids
Diagnosis
How do I know for sure that I have fibroids?
Your Minnesota Women's Care provider may find that you have fibroids when you have your regular pelvic exam (to check your uterus, ovaries, and vagina). Often, a health care provider will describe how small or large the fibroids are by comparing their size to the size your uterus would be if you were pregnant. For example, you may be told that your fibroids have made your uterus the size it would be if you were 8 weeks pregnant.
We can perform imaging tests, or tests that create a "picture" of the inside of your body without surgery, in order to confirm that you have fibroids. These tests might include:
- Ultrasound (which uses sounds waves to produce the picture)
- Magnetic Resonance Imaging (often called MRI) which uses magnets and radio waves to produce the picture
- X-rays (which use a form of radiation to see into the body and produce the picture)
- Cat scan or (CT scan) - which makes many pictures of the body from different angles to provide a more complete image.
Uterine Fibroids
FAQ
What causes fibroids?
No one knows for sure what causes fibroids. Researchers have some theories, but most likely, fibroids are the result of many factors interacting with each other. These factors could be hormonal (affected by estrogen levels), genetic (running in families), environmental, or a combination of all three. Because no one knows for sure what causes fibroids, we also don't know what causes them to grow or shrink. For the most part, fibroids stop growing or shrink after menopause. But, this is not true for all women with fibroids.
Can fibroids turn into cancer?
Fibroids are almost always benign, or not cancerous, and they rarely turn into cancer (less than 0.1 percent of cases). Having fibroids does not increase a woman's chances of getting cancer of the uterus.
Who gets fibroids?
Most of the time, fibroids grow in women of childbearing age. While no one knows for sure what will increase a woman's chances of getting fibroids, researchers have found that African American women are 2 to 3 times more likely to get them than women of other racial groups are. African American women also tend to get fibroids at a younger age than do other women with fibroids. Women who are overweight or obese also are at a slightly higher risk for fibroids than women who are not overweight. Women who have given birth appear to be at a lower risk for fibroids. Research is now being done to figure out who is at risk for fibroids.
Our Treatment Options
Treatment Options for Uterine Fibroids at Minnesota Women's Care
Surgical and Non-Surgical Options
There are many surgical and non-surgical treatment options for fibroids. The best treatment approach depends on many factors including what symptoms you are experiencing, the size number and location of the fibroids, and whether you are interested in pregnancy or not, among others. Your doctor will work with you to tailor the best treatment plan for you.
Understanding Your Surgical Treatment Options
There are many treatment options for fibroids that do not involve removing the uterus. If you want surgical treatment for your fibroids but don't want to undergo a hysterectomy, the procedures below are the ones we discuss with our patients at Minnesota Women's Care. There are a couple broad limitations to these approaches however:
- Since the uterus and often some fibroid tissue remains, there is always a chance the fibroids grow or return. Depending on the degree of growth, your symptoms may also return. The recurrence rates for each individual procedure are discussed below.
- Even though the uterus is spared, many of the procedures below disrupt the integrity of the uterine lining or blood flow which can make pregnancy high risk. The only procedure in which pregnancy is recommended after is a myomectomy. The others are technically for those who have completed childbearing.
Non-Surgical (Medical) Options for Fibroids
Hormonal and Non-Hormonal Medications
Combined estrogen-progestin contraceptives: These come in the form of a pill, patch, or ring, and known as traditional "OCPs." They are usually the first line approach, as can be used long-term, are well-tolerated, are relatively inexpensive, and provide contraception and additional benefits including decreasing the risk of ovarian and endometrial cancers.
Progestins: Options include high dose oral progestins (norethindrone acetate or medroxyprogesterone acetate most commonly), a progestin injection ("Depo provera," administered every 6 months), the etonorgestrel arm implant ("Nexplanon"), or the levonorgestrel intrauterine device (IUD). However, there is compelling evidence that the progesterone IUD results in a greater decrease in menstrual blood loss as compared to oral or other routes of administration.
One factor to note with progestins compared to OCPs is that while CHCs maintain a regular menses, continuous progestins can suppress periods completely (ie amenorrhea) or result in irregular bleeding. While this does not have negative long-term consequences (owing to its mechanism), it may be bothersome for some.
Gonadotropin-releasing hormone (Gn-RH) agonists and antagonists: These drugs block the production of ovarian-stimulating hormones, lowering estrogen levels. Since fibroids are estrogen responsive, this results in reduction of menstrual bleeding, and notably, some reduction in fibroid size. Because these drugs create an artificial menopause, one often experiences menopausal side effects such as hot flashes, sleep issues, and vaginal dryness. Some of the newer oral options mitigate this by including a low dose of estrogen and progestin added back within the medication.
There are currently two oral Gn-RH agonists on the market that are FDA approved for fibroid related heavy menstrual bleeding: Myfembree (relugolix-estradiol-norethindrone) and Orianhh (elagolix-estradiol-norethindrone). These medications have been found to result in a 50% reduction in menstrual blood loss, and can even improve bulk symptoms. However, due to limited data at this point they are both only approved for up to 24 months of use, and are not approved to be used as a contraceptive.
Tranexamic acid ("Lysteda"): This is a non-hormonal medication that works to slow down the breakdown of blood clots. In turn, slows down bleeding, and in this case can be used to reduce fibroid related bleeding. It is only taken during your period, rather than the entire month, and is non-hormonal; this makes it a good option for those who prefer to avoid contraception or a daily medication!
Uterine-sparing Surgical Options for Fibroids
Myomectomy
Essentially a myomectomy is a procedure where the fibroids are surgically removed from the uterus, and the uterine tissue is repaired. There are three ways to perform this procedure.
Hysteroscopic myomectomy: this is the least invasive option. With this approach, the surgeon enters the uterine cavity via the vagina/cervix with a small camera. When inside the uterus, they are able to remove the fibroids that line the endometrium, known as submucosal fibroids (see diagram below). Any intramural or subserosal fibroids cannot be accessed with this approach. For this reason, this procedure is good for you if you want a quick and simple procedure with very little recovery, and you have submucosal fibroids resulting in bleeding. If you have larger intramural or subserosal fibroids causing bulk symptoms, unfortunately this won't help.
Laparoscopic myomectomy: this where the surgeon enters the abdomen with a camera, and performs the surgery through small cuts. This is also a same day procedure and allows for a smooth recovery.
Abdominal myomectomy: this is the traditional way this procedure is performed, through a large incision. If the fibroids are numerous or very large, a laparoscopic approach is not feasible, and large cut has to be made. With this approach, you would stay in the hospital for at least one night, and the recovery is longer than the above two.
When performing a myomectomy, very small fibroids may not be visible and may be left behind. The growth of these fibroids is what contributes to the recurrence risk. In general, the rate of reoperation (ie sympoms returning and needing another surgery for fibroids) after 8 years is about 16%. The risk of recurrence is higher is one has multiple fibroids at time of surgery or if younger than 36 years old.
As above, if someone desires future pregnancy, a myomectomy is the only recommended surgical option. You need to discuss the risks with your provider.
Uterine Artery or Uterine Fibroid Embolization
This procedure is generally recommended for pre-menopausal people who have symptomatic fibroids (bleeding or bulky) and wish to retain their uterus but do not intend for future pregnancy. This procedure is performed by an interventional radiologist, rather than a gynecologist. The doctor inserts a catheter (a small tube) into a blood vessel and under image guidance, the catheter makes it way to the uterine blood vessels, which are then embolized. By blocking the blood supply to the fibroids, they shrink in size and symptoms improve. The procedure is done under sedation (rather than general anesthesia) and you go home the same day.
Outcomes of this procedure are generally favorable. In a large study, 70-90% of patients reported improvement or resolution in their heavy menstrual bleeding symptoms, and 80-90% reported improvement in their pain or bulk symptoms. The recurrence rate is worth noting however - after 5 years about 27% of patients end up needing a subsequent hysterectomy for failure or recurrence of symptoms.
NEW Surgical Treatment Now Available!
Radiofrequency fibroid ablation
Laparoscopic radiofrequency fibroid ablation (Lap-RFA, brand name Acessa) is a minimally invasive, energy-based treatment that reduces fibroid-related symptoms by reducing fibroid volume. This procedure is laparoscopic, meaning performed through several small incisions in the abdomen, and is performed on an outpatient basis with quick recovery. Return to normal activity is usually less than one week, which is a big advantage of this procedure.
During this procedure, the doctor visualizes the uterus with a camera and locates the fibroids using a laparoscopic ultrasound. After locating the fibroids, a device is used to heat up and destroy fibroid tissue. After one year, the size of the fibroid decreases by up to 66%, resulting in a significant reduction in pelvic pain, heavy periods, and bulk. As with any procedure that is uterine-sparing, there is always a risk of recurrent symptoms; for this procedure the rate of needing another surgery for fibroid-related symptoms was 11% at 3 years.
Pregnancy data on Lap-RFA is limited, as it is a newer technology and most studies have excluded patients planning for pregnancy. For this reason, should be used with caution if pregnancy is desired. That being said, case reports have reported favorable successful pregnancies after Lap-RFA, so hopefully more favorable data will continue to be collected.
In recent years the availability of Lap-RFA has been limited, particularly in the Midwest region. Minnesota Women's Care is now able to offer this life-changing option.
